The best feeling in the world is to be healthy. But it is not possible all the time to be healthy. Specially during this fast paced life. Everyone is in a hurry and busy without know “real” work. This unbalanced life is giving worth to so many fatal diseases. Here I am telling you some of the most deadly diseases throughout the world. The Common Cold
 The common cold (also known as nasopharyngitis, rhinopharyngitis, acute coryza, or a cold) is a viral infectious disease of the upper respiratory system which affects primarily the nose. Symptoms include a cough, sore throat, runny nose, and fever which usually resolve in seven to ten days, with some symptoms lasting up to three weeks. Well over 200 viruses are implicated in the cause of the common cold; the rhinoviruses are the most common.
The common cold (also known as nasopharyngitis, rhinopharyngitis, acute coryza, or a cold) is a viral infectious disease of the upper respiratory system which affects primarily the nose. Symptoms include a cough, sore throat, runny nose, and fever which usually resolve in seven to ten days, with some symptoms lasting up to three weeks. Well over 200 viruses are implicated in the cause of the common cold; the rhinoviruses are the most common.
Upper respiratory tract infections are loosely divided by the areas they affect, with the common cold primarily affecting the nose, the throat (pharyngitis), and the sinuses (sinusitis). Symptoms are mostly due to the body’s immune response to the infection rather than to tissue destruction by the viruses themselves. The primary method of prevention is by hand washing with some evidence to support the effectiveness of wearing face masks.
No cure for the common cold exists, but the symptoms can be treated. It is the most frequent infectious disease in humans with the average adult contracting two to three colds a year and the average child contracting between six and twelve. These infections have been with humanity since antiquity.
Cancer
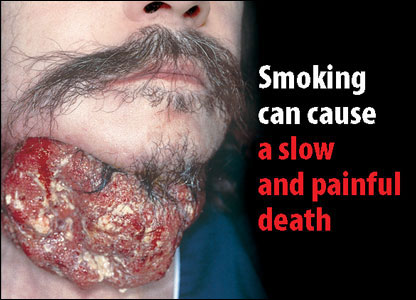 Cancer known medically as a malignant neoplasm, is a broad group of various diseases, all involving unregulated cell growth. In cancer, cells divide and grow uncontrollably, forming malignant tumors, and invade nearby parts of the body. The cancer may also spread to more distant parts of the body through the lymphatic system or bloodstream. Not all tumors are cancerous. Benign tumors do not grow uncontrollably, do not invade neighboring tissues, and do not spread throughout the body.
Cancer known medically as a malignant neoplasm, is a broad group of various diseases, all involving unregulated cell growth. In cancer, cells divide and grow uncontrollably, forming malignant tumors, and invade nearby parts of the body. The cancer may also spread to more distant parts of the body through the lymphatic system or bloodstream. Not all tumors are cancerous. Benign tumors do not grow uncontrollably, do not invade neighboring tissues, and do not spread throughout the body.
Determining what causes cancer is complex. Many things are known to increase the risk of cancer, including tobacco use, certain infections, radiation, lack of physical activity, poor diet and obesity, and environmental pollutants. These can directly damage genes or combine with existing genetic faults within cells to cause the disease.
Approximately five to ten percent of cancers are entirely hereditary.
Cancer can be detected in a number of ways, including the presence of certain signs and symptoms, screening tests, or medical imaging. Once a possible cancer is detected it is diagnosed by microscopic examination of a tissue sample. Cancer is usually treated with chemotherapy, radiation therapy and surgery.
The chances of surviving the disease vary greatly by the type and location of the cancer and the extent of disease at the start of treatment. While cancer can affect people of all ages, and a few types of cancer are more common in children, the risk of developing cancer generally increases with age. In 2007, cancer caused about 13% of all human deaths worldwide (7.9 million). Rates are rising as more people live to an old age and as mass lifestyle changes occur in the developing world.
Asthma
Asthma (from the Greek άσθμα, ásthma, “panting”) is the common chronic inflammatory disease of the airways characterized by variable and recurring symptoms, reversible airflow obstruction, and bronchospasm. Symptoms include wheezing, coughing, chest tightness, and shortness of breath.[2] Asthma is clinically classified according to the frequency of symptoms, forced expiratory volume in 1 second (FEV1), and peak expiratory flow rate. Asthma may also be classified as atopic (extrinsic) or non-atopic (intrinsic).
It is thought to be caused by a combination of genetic and environmental factors. Treatment of acute symptoms is usually with an inhaled short-acting beta-2 agonist (such as salbutamol). Symptoms can be prevented by avoiding triggers, such as allergens and irritants, and by inhaling corticosteroids. Leukotriene antagonists are less effective than corticosteroids and thus less preferred.
Its diagnosis is usually made based on the pattern of symptoms and/or response to therapy over time. The prevalence of asthma has increased significantly since the 1970s. As of 2010, 300 million people were affected worldwide. In 2009 asthma caused 250,000 deaths globally. Despite this, with proper control of asthma with step down therapy, prognosis is generally good.
HIV/AIDS

Human immunodeficiency virus (HIV) is a lentivirus (a member of the retrovirus family) that causes acquired immunodeficiency syndrome (AIDS), a condition in humans in which progressive failure of the immune system allows life-threatening opportunistic infections and cancers to thrive. Infection with HIV occurs by the transfer of blood, semen, vaginal fluid, pre-ejaculate, or breast milk.
Within these bodily fluids, HIV is present as both free virus particles and virus within infected immune cells. The four major routes of transmission are unsafe sex, contaminated needles, breast milk, and transmission from an infected mother to her baby at birth (perinatal transmission). Screening of blood products for HIV has largely eliminated transmission through blood transfusions or infected blood products in the developed world.
HIV infection in humans is considered pandemic by the World Health Organization (WHO). Nevertheless, complacency about HIV may play a key role in HIV risk. From its discovery in 1981 to 2006, AIDS killed more than 25 million people. HIV infects about 0.6% of the world’s population.
In 2009, AIDS claimed an estimated 1.8 million lives, down from a global peak of 2.1 million in 2004. Approximately 260,000 children died of AIDS in 2009. A disproportionate number of AIDS deaths occur in Sub-Saharan Africa, retarding economic growth and exacerbating the burden of poverty.
An estimated 22.5 million people (68% of the global total) live with HIV in sub-Saharan Africa, which is also home to 90% of the world’s 16.6 million children orphaned by HIV. Treatment with antiretroviral drugs reduces both the mortality and the morbidity of HIV infection.
Although antiretroviral medication is still not universally available, expansion of antiretroviral therapy programs since 2004 has helped to turn the tide of AIDS deaths and new infections in many parts of the world. Intensified awareness and preventive measures, as well as the natural course of the epidemic, have also played a role. Nevertheless, an estimated 2.6 million people were newly infected in 2009.
HIV infects vital cells in the human immune system such as helper T cells (specifically CD4+ T cells), macrophages, and dendritic cells. HIV infection leads to low levels of CD4+ T cells through three main mechanisms: First, direct viral killing of infected cells; second, increased rates of apoptosis in infected cells; and third, killing of infected CD4+ T cells by CD8 cytotoxic lymphocytes that recognize infected cells.
When CD4+ T cell numbers decline below a critical level, cell-mediated immunity is lost, and the body becomes progressively more susceptible to opportunistic infections.
Most untreated people infected with HIV-1 eventually develop AIDS. These individuals mostly die from opportunistic infections or malignancies associated with the progressive failure of the immune system. HIV progresses to AIDS at a variable rate affected by viral, host, and environmental factors; most will progress to AIDS within 10 years of HIV infection: some will have progressed much sooner, and some will take much longer.
Treatment with anti-retrovirals increases the life expectancy of people infected with HIV. Even after HIV has progressed to diagnosable AIDS, the average survival time with antiretroviral therapy was estimated to be more than 5 years as of 2005. Without antiretroviral therapy, someone who has AIDS typically dies within a year.
Diabetes
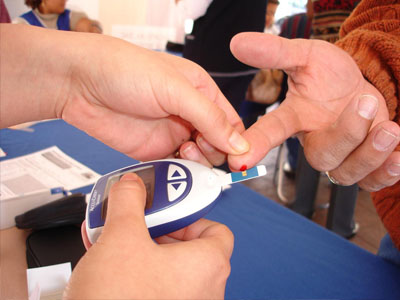
Diabetes mellitus, often simply referred to as diabetes, is a group of metabolic diseases in which a person has high blood sugar, either because the body does not produce enough insulin, or because cells do not respond to the insulin that is produced. This high blood sugar produces the classical symptoms of polyuria (frequent urination), polydipsia (increased thirst) and polyphagia (increased hunger).
The three main types of diabetes mellitus (DM) are:
- Type 1 DM results from the body’s failure to produce insulin, and presently requires the person to inject insulin. (Also referred to as insulin-dependent diabetes mellitus (IDDM) or “juvenile” diabetes)
- Type 2 DM results from insulin resistance, a condition in which cells fail to use insulin properly, sometimes combined with an absolute insulin deficiency. (Formerly referred to as noninsulin-dependent diabetes mellitus (NIDDM) or “adult-onset” diabetes)
- Gestational diabetes is when pregnant women, who have never had diabetes before, have a high blood glucose level during pregnancy. It may precede development of type 2 DM.
Other forms of diabetes mellitus include congenital diabetes, which is due to genetic defects of insulin secretion, cystic fibrosis-related diabetes, steroid diabetes induced by high doses of glucocorticoids, and several forms of monogenic diabetes.
All forms of diabetes have been treatable since insulin became available in 1921, and type 2 diabetes may be controlled with medications. Both types 1 and 2 are chronic conditions that usually cannot be cured.
Pancreas transplants have been tried with limited success in type 1 DM; gastric bypass surgery has been successful in many with morbid obesity and type 2 DM. Gestational diabetes usually resolves after delivery. Diabetes without proper treatments can cause many complications. Acute complications include hypoglycemia, diabetic ketoacidosis, or nonketotic hyperosmolar coma.
Serious long-term complications include cardiovascular disease, chronic renal failure, and diabetic retinopathy (retinal damage). Adequate treatment of diabetes is thus important, as well as blood pressure control and lifestyle factors such as smoking cessation and maintaining a healthy body weight.Globally as of 2010, an estimated 285 million people have type 2 diabetes, making up about 90% of all diabetes cases.
Creutzfeldt-Jakob Disease
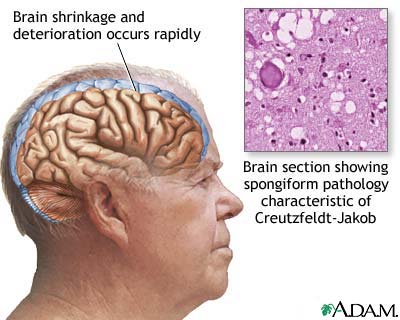
Creutzfeldt–Jakob disease or CJD is a degenerative neurological disorder (brain disease) that is incurable and invariably fatal. CJD is at times called a human form of mad cow disease even though classic CJD is not related to bovine spongiform encephalopathy, however, given that bovine spongiform encephalopathy is believed to be the cause of variant Creutzfeldt–Jakob (vCJD) disease in humans, the two are often confused.
Variant CJD (vCJD) is the most common among the types of transmissible spongiform encephalopathy found in humans. In CJD, the brain tissue develops holes and takes on a sponge-like texture. This is due to a type of infectious protein called a prion. Prions are misfolded proteins which replicate by converting their properly folded counterparts.
Creutzfeldt–Jakob disease or CJD is a degenerative neurological disorder (brain disease) that is incurable and invariably fatal. CJD is at times called a human form of mad cow disease even though classic CJD is not related to bovine spongiform encephalopathy, however, given that bovine spongiform encephalopathy is believed to be the cause of variant Creutzfeldt–Jakob (vCJD) disease in humans, the two are often confused.
Variant CJD (vCJD) is the most common among the types of transmissible spongiform encephalopathy found in humans. In CJD, the brain tissue develops holes and takes on a sponge-like texture. This is due to a type of infectious protein called a prion. Prions are misfolded proteins which replicate by converting their properly folded counterparts.
The disease was first described in the 1920s by the German neurologists Hans Gerhard Creutzfeldt and Alfons Maria Jakob. Creutzfeldt-Jakob disease is similar to other neurodegenerative diseases such as kuru, a human disorder, and scrapie, which occurs in sheep and goats. All three diseases are types of transmissible spongiform encephalopathies, so called because of the characteristic spongelike pattern of neuronal destruction that leaves brain tissue filled with holes.
Influenza
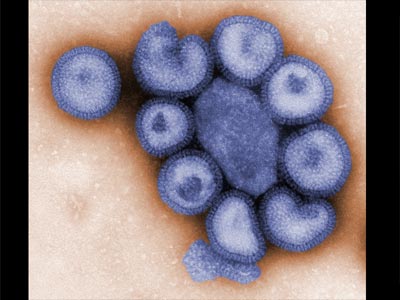
Influenza, commonly referred to as the flu, is an infectious disease caused by RNA viruses of the family Orthomyxoviridae (the influenza viruses), that affects birds and mammals. The most common symptoms of the disease are chills, fever, sore throat, muscle pains, severe headache, coughing, weakness/fatigue and general discomfort.
Although it is often confused with other influenza-like illnesses, especially the common cold, influenza is a more severe disease than the common cold and is caused by a different type of virus. Influenza may produce nausea and vomiting, particularly in children, but these symptoms are more common in the unrelated gastroenteritis, which is sometimes, inaccurately, referred to as “stomach flu.” Flu can occasionally cause either direct viral pneumonia or secondary bacterial pneumonia.
Typically, influenza is transmitted through the air by coughs or sneezes, creating aerosols containing the virus. Influenza can also be transmitted by direct contact with bird droppings or nasal secretions, or through contact with contaminated surfaces.
Airborne aerosols have been thought to cause most infections, although which means of transmission is most important is not absolutely clear. Influenza viruses can be inactivated by sunlight, disinfectants and detergents. As the virus can be inactivated by soap, frequent hand washing reduces the risk of infection.
Influenza spreads around the world in seasonal epidemics, resulting in the deaths of between 250,000 and 500,000 people every year, up to millions in some pandemic years. On average 41,400 people died each year in the United States between 1979 and 2001 from influenza. In 2010 the Centers for Disease Control and Prevention (CDC) in the United States changed the way it reports the 30 year estimates for deaths. Now they are reported as a range from a low of about 3,300 deaths to a high of 49,000 per year.
Three influenza pandemics occurred in the 20th century and killed tens of millions of people, with each of these pandemics being caused by the appearance of a new strain of the virus in humans. Often, these new strains appear when an existing flu virus spreads to humans from other animal species, or when an existing human strain picks up new genes from a virus that usually infects birds or pigs.
An avian strain named H5N1 raised the concern of a new influenza pandemic, after it emerged in Asia in the 1990s, but it has not evolved to a form that spreads easily between people. In April 2009 a novel flu strain evolved that combined genes from human, pig, and bird flu, initially dubbed “swine flu” and also known as influenza A/H1N1, emerged in Mexico, the United States, and several other nations.
The World Health Organization officially declared the outbreak to be a pandemic on June 11, 2009 (see 2009 flu pandemic). The WHO’s declaration of a pandemic level 6 was an indication of spread, not severity, the strain actually having a lower mortality rate than common flu outbreaks.
Vaccinations against influenza are usually made available to people in developed countries. Farmed poultry is often vaccinated to avoid decimation of the flocks. The most common human vaccine is the trivalent influenza vaccine (TIV) that contains purified and inactivated antigens against three viral strains.
Typically, this vaccine includes material from two influenza A virus subtypes and one influenza B virus strain. The TIV carries no risk of transmitting the disease, and it has very low reactivity. A vaccine formulated for one year may be ineffective in the following year, since the influenza virus evolves rapidly, and new strains quickly replace the older ones.
Antiviral drugs such as the neuraminidase inhibitor oseltamivir have been used to treat influenza; however, their effectiveness is difficult to determine due to much of the data remaining unpublished.
Lupus Erythematosus
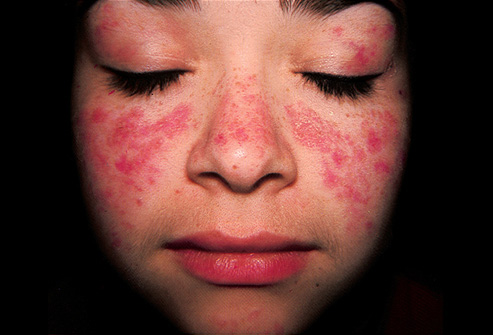
Lupus erythematosus is a category for a collection of diseases with similar underlying problems with immunity (autoimmune disease). Symptoms of these diseases can affect many different body systems, including joints, skin, kidneys, blood cells, heart, and lungs.
Four main types of lupus exist: systemic lupus erythematosus, discoid lupus erythematosus, drug-induced lupus erythematosus, and neonatal lupus erythematosus. Of these, systemic lupus erythematosus (also known as SLE) is the most common and serious form of lupus.
Lupus is an autoimmune disease where the body’s immune system becomes hyperactive and attacks normal, healthy tissue. When the body’s immune system is operating normally it produces antibodies to fight viruses and bacteria and other antigens.
Lupus makes the antibodies created unable to differentiate between antigens and healthy tissue causing the antibodies to attack healthy tissue. Resulting symptoms include inflammation, swelling, damage to joints, skin, kidneys, blood, heart and lungs.
Photosensitivity’s relationship to and influence on the systemic manifestations of lupus remain to be defined. Mechanisms for photosensitivity might include: modulation of autoantibody location, cytotoxic effects, apoptosis induction with autoantigens in apoptotic blebs, upregulation of adhesion molecules and cytokines, induction of nitric oxide synthase expression and ultraviolet-generated antigenic DNA. Tumor necrosis factor alpha also seems to play a role in the development of photosensitivity.
Polio
Poliomyelitis often called polio or infantile paralysis, is an acute, viral, infectious disease spread from person to person, primarily via the fecal-oral route. The term derives from the Greek poliós (πολιός), meaning “grey”, myelós (µυελός), referring to the “spinal cord”, and the suffix -itis, which denotes inflammation.
Although approximately 90% of polio infections cause no symptoms at all, affected individuals can exhibit a range of symptoms if the virus enters the blood stream. In about 1% of cases, the virus enters the central nervous system, preferentially infecting and destroying motor neurons, leading to muscle weakness and acute flaccid paralysis.
Different types of paralysis may occur, depending on the nerves involved. Spinal polio is the most common form, characterized by asymmetric paralysis that most often involves the legs. Bulbar polio leads to weakness of muscles innervated by cranial nerves. Bulbospinal polio is a combination of bulbar and spinal paralysis.
Poliomyelitis was first recognized as a distinct condition by Jakob Heine in 1840. Its causative agent, poliovirus, was identified in 1908 by Karl Landsteiner.
Although major polio epidemics were unknown before the late 19th century, polio was one of the most dreaded childhood diseases of the 20th century. Polio epidemics have crippled thousands of people, mostly young children; the disease has caused paralysis and death for much of human history. Polio had existed for thousands of years quietly as an endemic pathogen until the 1880s, when major epidemics began to occur in Europe; soon after, widespread epidemics appeared in the United States.
By 1910, much of the world experienced a dramatic increase in polio cases and epidemics became regular events, primarily in cities during the summer months. These epidemics—which left thousands of children and adults paralyzed—provided the impetus for a “Great Race” towards the development of a vaccine.
Developed in the 1950s, polio vaccines are credited with reducing the global number of polio cases per year from many hundreds of thousands to today under a thousand. Enhanced vaccination efforts led by the World Health Organization, UNICEF, and Rotary International could result in global eradication of the disease.
Ebola
Ebola is a virus of the family Filoviridae that is responsible for a severe and often fatal viral hemorrhagic fever; outbreaks in primates such as gorillas and chimpanzees as well as humans have been recorded. The disease is characterized by extreme fever, rash, and profuse hemorrhaging. In humans, fatality rates range from 50 to 90 percent.
The virus takes its name from the Ebola River in the northern Congo basin of central Africa, where it first emerged in 1976. Outbreaks that year in Zaire (now Congo [Kinshasa]) and The Sudan resulted in hundreds of deaths, as did another outbreak in Zaire in 1995. Ebola is closely related to the Marburg virus, which was discovered in 1967, and the two are the only members of the Filoviridae that cause epidemic human disease. A third related agent, called Ebola Reston, caused an epidemic in laboratory monkeys in Reston, Virginia, but apparently is not fatal to humans.









One Response
Hmm is anyone else encountering problems with the images on this blog loading?
I’m trying to figure out if its a problem on my end or if it’s the blog.
Any feed-back would be greatly appreciated.